About the research
Secondhand smoke is still a major cause of death and ill-health Internationally. Analysis by Öberg et al suggests that it causes nearly 600,000 deaths and approaching 11,000,000 disability-adjusted life years annually. In their Framework Convention on Tobacco Control, the World Health Organisation includes this key principle in article 8: “all people should be protected from exposure to tobacco smoke”
During the past decade many developed countries have introduced legislation to reduce smoking in workplaces and other enclosed public spaces, which has been shown to lower amounts of secondhand smoke, protecting workers and non-smokers. However, the legislation has generally not included homes and other private spaces.
To examine the level of exposure to secondhand smoke in non-smoking adults living in Scotland, data from the Scottish Health Survey was analysed. The Scottish Health Survey provides a rich source of population data and has been conducted eleven times from 1995 to 2016, with a sample size in the range of 4000-900 adults. The 2015 Scottish Health Survey report included summary details of salivary cotinine concentrations for all non-smoking adults who provided a valid saliva sample between 2003 and 2015.
The report produced a geometric mean for all samples from non-smoking adults which were below a value of 0.05ng/mL (representing half the analytical method limit of detection (limit of detection=0.1ng/ mL).
How to handle highly skewed, left-censored data such as these is an issue of debate in the exposure science community, especially where there is a substantial proportion of non-detects. Censoring in data is a condition in which the value of a measurement or observation is only partially known. Using half the limit of detection rather than using undetectable values results in positively biased estimates of average exposure.
Policymakers and other stakeholders need reliable and understandable information on exposure to secondhand smoke if they are to decide on the correct approach to protect populations from harm by it. Such information needs to stand in the context of changes over time of population exposure to secondhand smoke in countries which are attempting to ultimately eliminate tobacco use.
Using the analysis of salivary cotinine data from subsamples of the non-smoking adults collected in the Scottish Health Survey since 1998, the research aimed to produce two useful metrics of population exposure:
- the proportion of non-smokers with non-measurable cotinine
- calculation of the population geographic mean based on a statistical methodology that takes account of undetectable cotinine levels.
Research funding and partners
Research undertaken as part of employment at the Universities of Stirling and Aberdeen (Sean Semple), Glasgow (Alastair H Leyland and Linsay Gray) and Heriot Watt (John W Cherrie). Linsay Gray and Alastair H Leyland receive core funding from the Medical Research Council (MC_UU_12017/13) and the Scottish Government Chief Scientist Office (SPHSU13).
Key message
There has been a significant decrease in measurable exposure to secondhand smoke in Scotland since the introduction of smoke-free legislation.
Methodology
The research used data from the Scottish Health Survey – a nationally representative sample of household population in Scotland – from 1998 to 2016, obtained from the UK Data Service.
The data covered people who were 16 or older and who had a valid cotinine sample below 12ng/mL, the cut-off point for validated non-smoking adults. The total sample size was 13563, ranging from 630 non-smoking adults in 2015 to 3738 in 1998. For each time point, the proportion of valid samples below 0.1ng/mL (the limit of detection) for salivary cotinine was calculated.
Owing to the low levels of cotinine reported in the Scottish Health Survey samples, with a high proportion being below the limit of detection, arithmetic mean, media and mode were identified as suitable tools for describing exposures in the data. The geometric mean is most commonly used in these cases but as 0 value data cannot be included, it is often necessary to impute values for samples below the limit of detection. In the 2015 Scottish Health Survey, the geometric mean salivary cotinine was reported as 0.09 ng/mL. The value was derived because over three-quarters of the sample provided saliva with cotinine below the limit of detection. In such cases, the samples were assigned a value of 0.05 ng/mL, on the basis of it being halfway between 0 and the limit of detection of 0.1 ng/mL, in accordance with traditional practice.
Geometric mean and 95% confidence intervals were calculated using Tobit regression oflog-transformed concentrations with the limit of detection as the lower limit. The Tobit model is a statistical model proposed by James Tobin (1958) to describe the relationship between a non-negative dependent variable and an independent variable (or vector). The model is a recommended method for datasets containing values below detection and has been used in other research on tobacco smoking.
After the data had been extracted from the original SPSS V.19.0 files downloaded from the UK Data Service, analysis was performed in Microsoft Excel and Stata V.13.1. Change was calculated for the whole period 1998–2016. Smoke-free legislation was brought into force in Scotland in 2006, so the trend in the data available for this period (2008–2016) was assessed by utilising a linear best-fit line and determining the regression equation.
During the period analysed, the sample calculation method did not change. Since 2009, the method used for the Scottish Health Survey to analyse saliva samples has been high-performance liquid chromatography coupled to tandem mass spectrometry with multiple reaction monitoring (LC-MS), as opposed to the gas chromatography nitrogen phosphorous detection method used in the 1998, 2003 and 2008 surveys. Prior to LC-MS, the sample preparation was liquid/liquid extraction. Throughout the period covered by this research, the limit of detection has not changed.
The study did not analyse the sociodemographic patterning of salivary cotinine concentrations. However, the 2016 Scottish Health Survey demonstrates a gradient in self-reported exposure to secondhand smoke: in the 20% most deprived homes, 64% of non-smoking adults reported exposure to secondhand smoke, while in the 20% most affluent areas, 75% of non-smoking adults reported no exposure.
Messages
There has been a significant decrease in measurable exposure to secondhand smoke in Scotland since the introduction of smoke-free legislation.
Findings
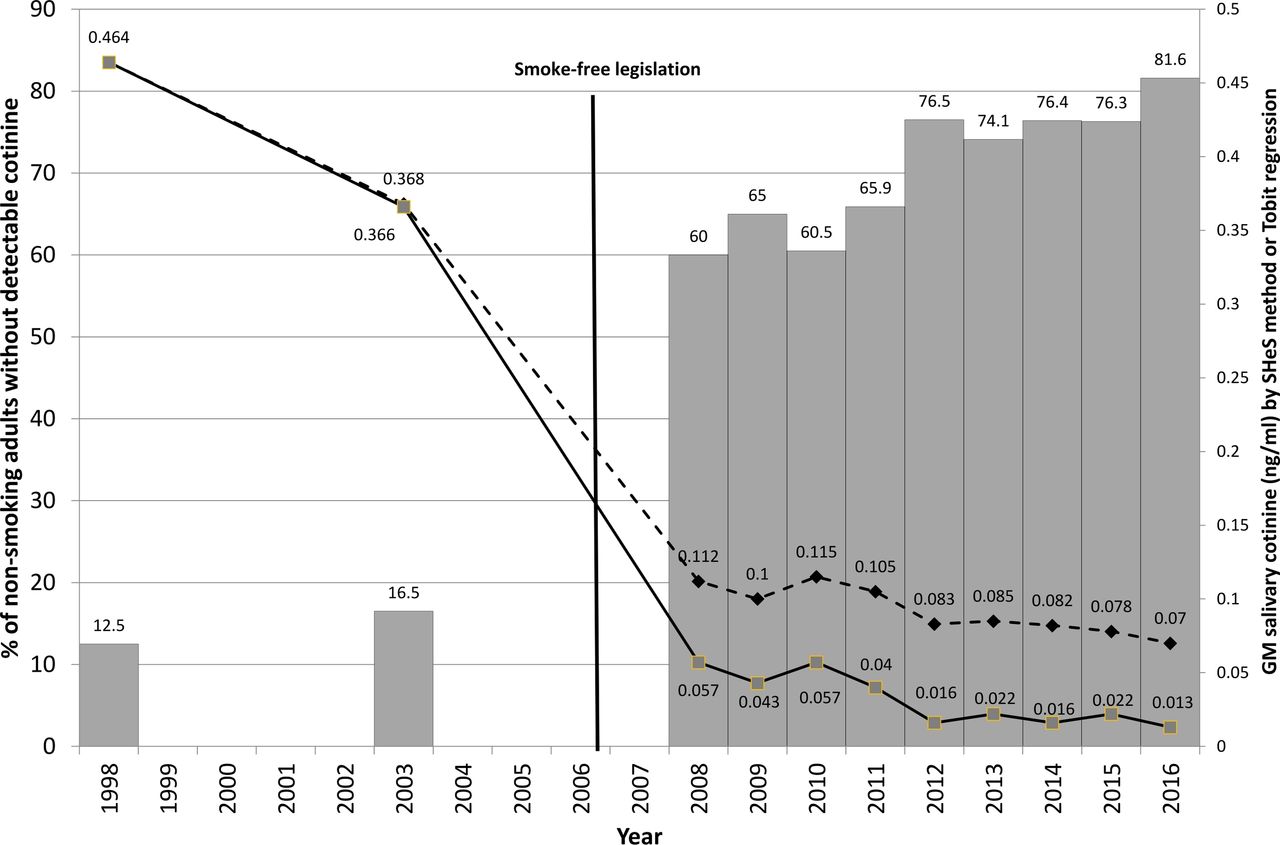
Figure 1 shows details of the salivary cotinine data for non-smoking adults in Scotland from the Scottish Health Surveys between 1998 and 2016.
Figure 1: Scottish Health Survey salivary cotinine data from non-smoking adults 1998–2016. The bars represent the percentage of non-smoking adults with non-detectable cotinine, the dashed line shows the geometric mean value calculated by the previous methodology using one-half the limit of detection; the solid line shows the geometric mean value calculated using Tobit regression.
Image from Semple S, Mueller W, Leyland AH, et al, Assessing progress in protecting non-smokers from secondhand smoke. Tobacco Control.
Published Online First: 29 August 2018. doi: 10.1136/tobaccocontrol-2018-054599.
Reproduced under the Creative Commons Attribution 4.0 Unported (CC BY 4.0) license.
Click on figure to download larger version.
The researchers noted an increase in percentage of non-smoking adults who had no detectable cotinine in their saliva the from 12.5% (95% confidence interval 11.5% to 13.6%) in 1998 to 81.6% (95% confidence interval 78.6% to 84.6%) in 2016. During this period, the figures demonstrate a more than sixfold increase in the proportion of non-smokers protected from the harm of secondhand smoke.
Expressed as a geometric mean, determined from Tobit regression, the population exposure also reduced significantly from 0.464ng/mL (95% confidence interval 0.444 to 0.486ng/mL) in 1998 to 0.013ng/mL (95% confidence interval 0.009 to 0.020ng/mL) in 2016: a reduction of 97.2%.
Compared to the figures derived from the previous methodology for the period following smoke-free legislation in Scotland, Tobit regression-based estimates were lower by around 0.05ng/mL. The reduction mostly occurs during the period from 2003 to 2008. Restrictions on smoking in enclosed public spaces (nearly all work and leisure spaces) were introduced in March 2006 in Scotland.
Restricting the analysis to the years 2008 to 2016 (after the introduction of smoke-free legislation), the results show continued improvements in the proportion of adults without measurable cotinine (from 60.0% in 2008 to 81.6% in 2016) by 2.67% per annum (R2=0.85).There was a similar reduction in the geometric mean of salivary cotinine concentrations from 0.057ng/mL (95% confidence interval 0.047 to 0.070) in 2008 to 0.013ng/mL (95% confidence interval 0.009 to 0.020) in 2016: a reduction of −0.006ng/mL per annum (R2=0.76).
The Scottish Health Survey for 2012–2016 included non-smoking adults’ self-reporting on whether they perceived themselves to be exposed to secondhand smoke in a range of locations:
- in their own or other people’s homes
- at work
- in cars/vans
- in other public spaces.
For each of the 2012 to 2014 surveys, 70% of non-smoking adults reported that they had not been exposed to smoke in any of these places. By the time of the 2015 survey, the number of those self-reporting had risen to 74% and by 2016 the figure was 73%. These figures are broadly in line with the proportion of non-smoking adults with no measurable salivary cotinine identified by this research.
The research demonstrates that there have been very large reductions in Scottish non-smoking adults’ exposure to secondhand smoke.
The research is based on data where a high proportion of the cotinine samples are below the level of detection. Consequently, further improvements in the techniques used in chemical analysis of the samples could increase the reliability of the measures of change in exposure to secondhand smoke. Additionally, the Tobit Regression methods used in this research could be further developed to explore the effects of exposure to secondhand smoke based on factors such as living with a smoker or occupational exposure.
While the research demonstrates that considerable improvements have been made in Scotland towards reducing exposure to secondhand smoke, the results also show that nearly a fifth of Scottish non-smoking adults remain exposed to it on a regular basis.
The research also demonstrates that exposure to secondhand smoke remains a public health issue. Further measures by the public health community, building on their current efforts will be needed to continue the reduction in exposure to secondhand smoke. Objective measurements, such as salivary cotinine, and the development of further targets by policy-makers will be needed to further the control of tobacco and secondhand smoke.
Findings for policy
The research provides evidence to help demonstrate the positive impacts of smoke-free legislation which has already been implemented, as well as providing additional evidence for policymakers working to reduce smoking further.
The results of this research mirror those of research done in England using the Health Survey for England on children’s exposure to secondhand smoke:
Jarvis MJ, Feyerabend C. Recent trends in children’s exposure to secondhand smoke in England: cotinine evidence from the Health Survey for England. Addiction 2015;110:1484–92, https://doi.org/10.1111/add.12962
Impact
The research is being utilised by public health charities such as ASH Scotland to promote the value of policies and campaigns focused on reducing smoking. Sheila Duffy, Chief Executive of ASH Scotland, welcomed the findings. She said: “It is established scientific fact that second-hand tobacco smoke is harmful to health and is associated with a range of illnesses. So I am delighted to see the huge reductions in second-hand smoke exposure in Scotland, delivering a healthier living environment to nearly half the population of Scotland. This has not happened by accident but is the result of deliberate and sustained work by successive Scottish administrations and is a clear example of the benefits of public health campaigns.” (quote via University of Stirling news item)
Media coverage
Second-hand smoke exposure falls by 97 per cent over 20 years, The Scotsman, 3 Sep 2018
Dramatic fall in second-hand smoke exposure, study finds, ITV News, 3 Sep 2018
Passive smoking almost eradicated, The Times, 4 Sep 2018
Publications
UK Data Service Data Impact blog post: Much ado about next to nothing